Physiotherapy for Sciatic Pain: Your Path to Relief
Sciatic Pain Physiotherapy: What to Expect
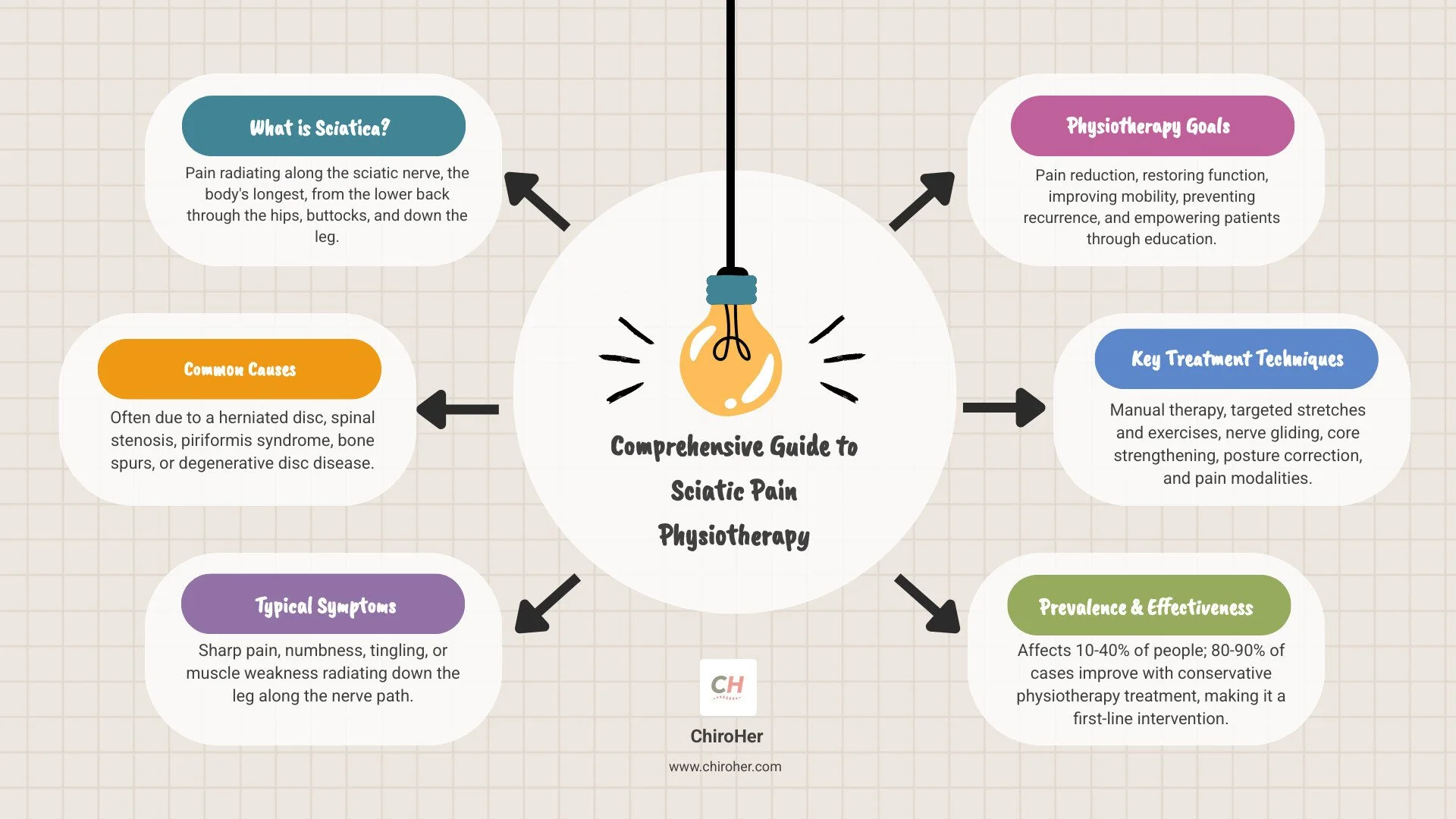
Sciatic pain physiotherapy offers an effective, non-invasive approach for a common type of nerve pain. This targeted approach combines exercises, manual therapy, and lifestyle changes to address the root causes of sciatic nerve irritation.
Key physiotherapy approaches for sciatic pain include:
Manual therapy and joint mobilization
Targeted stretching for the piriformis, hamstring, and hip flexors
Core strengthening exercises for spinal stability
Nerve gliding techniques to improve nerve mobility
Posture correction and ergonomic education
Pain management with heat, cold, or TENS units
Sciatica affects 10-40% of people, with pain radiating along the sciatic nerve from the lower back down the leg. Research shows 80-90% of cases improve with conservative care, making physiotherapy a first-line intervention. This active, educational approach aims to provide pain relief and empowers you to manage your recovery and reduce the risk of future episodes.
Hi! I'm Dr. Michelle Andrews, and I've worked with hundreds of patients in Oklahoma City to help manage sciatic pain. My experience with sciatic pain physiotherapy shows that combining manual therapy, targeted exercises, and patient education can lead to lasting results.
Your Comprehensive Guide to Sciatic Pain Physiotherapy
When sharp, shooting pain radiates down your leg, it's tempting to rest. However, my experience shows that sciatic pain physiotherapy works best with movement, not avoidance. Physiotherapy is an active, educational approach. Instead of masking symptoms, we work to identify and address the root cause to reduce the risk of recurrence, empowering you to control your recovery.
At ChiroHer, our sciatic pain physiotherapy program focuses on four goals: pain management, restoring function, improving mobility, and reducing the risk of recurrence. We strengthen your core, improve flexibility, and teach you proper movement patterns to protect your sciatic nerve.
Our emphasis on patient education means you'll understand what's happening in your body and learn strategies to manage symptoms at home, giving you a toolkit for long-term wellness.
Common Causes and Symptoms of Sciatica
Sciatica is a symptom, not a condition. It's your body's alarm that the sciatic nerve (the longest in your body) is compressed or irritated.
Common causes include:
Herniated discs: The cause of about 90% of cases, where the soft center of a spinal disc presses on a nerve root.
Spinal stenosis: A narrowing of the spinal canal that compresses the nerve.
Piriformis syndrome: A spasm or tightening of a deep buttock muscle that irritates the nearby sciatic nerve, which I often see in patients who sit for long periods.
Other causes can be bone spurs, degenerative disc disease, spondylolisthesis, pregnancy, or trauma. Symptoms vary but often include sharp, shooting pain, a dull ache, numbness, tingling, or muscle weakness in the leg. The specific symptoms help guide our approach, as confirmed by scientific research on sciatica causes.
The Goals of a Sciatic Pain Physiotherapy Program
A primary goal is to help you move with greater comfort. Sciatic pain physiotherapy aims for lasting change, not just temporary symptom management. Our program focuses on:
Pain management: We use targeted techniques to address inflammation and centralize pain by moving it from your leg toward your spine, a positive sign of improvement.
Core strengthening: A strong core, including your back, abdomen, and hip muscles, supports your spine and takes pressure off the sciatic nerve.
Improved flexibility: We lengthen tight muscles like the hamstrings and piriformis that can contribute to nerve compression.
Better posture: We teach you how to sit, stand, and move to protect your spine from uneven pressure.
Reducing recurrence: The strength and knowledge you gain are your best defense against future sciatic pain.
Key Physiotherapy Techniques for Sciatica Relief
Because every case of sciatica is unique, our sciatic pain physiotherapy approach combines multiple techniques customized to your needs. Our toolkit includes:
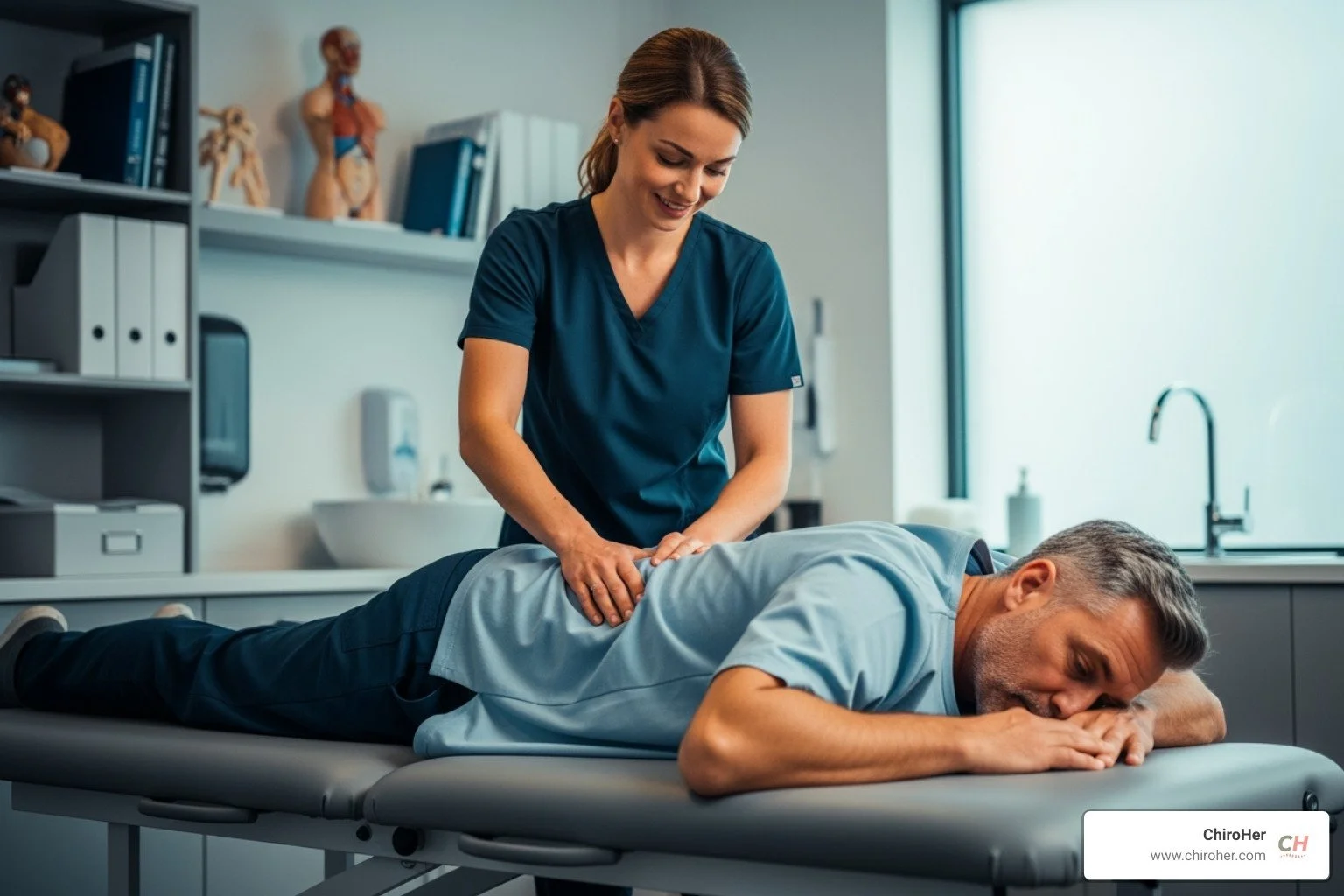
Manual therapy: Hands-on techniques like joint mobilization and soft tissue massage reduce pressure on nerve roots and release tight muscles.
Nerve gliding exercises: These specific movements help the sciatic nerve slide smoothly, which may reduce tingling and numbness.
The McKenzie Method: We use directional movements to identify exercises that centralize your pain, moving it from the leg toward the spine.
Therapeutic exercise: We go beyond stretching to include core strengthening, endurance training, and gait training to correct movement patterns.
Pain management: We may use TENS units, heat and cold therapy, or dry needling to manage pain and muscle spasms.
Posture and ergonomic education: We help you identify and fix problematic patterns in your daily activities, from your workspace to your sleeping position.
Our holistic wellness services complement these techniques, addressing your whole person.
Stretches and Exercises to Manage Pain
Movement can be beneficial for sciatica. Gentle, targeted exercises promote recovery and help prevent the stiffness that comes from inactivity. Try these movements, but never force anything that increases your pain.
Knee-to-chest stretch: Lie on your back, bring one knee to your chest, and hold for 20-30 seconds. This lengthens lower back muscles.
Seated piriformis stretch: In a chair, place your ankle on the opposite knee. Gently lean forward with a straight back and hold for 20-30 seconds.
Standing hamstring stretch: Place your heel on a step, keep the leg straight, and lean forward from your hips. Hold for 15-30 seconds.
Glute bridges: Lie on your back with knees bent. Lift your hips to form a straight line from shoulders to knees. Hold briefly and lower slowly.
Pelvic tilts: Lie on your back with knees bent. Tighten your abs to flatten your lower back against the floor. Hold for 5-10 seconds.
Sciatic nerve glides: Lie on your back and lift your leg with the knee bent. Slowly straighten the knee while flexing your ankle, then reverse.
These movements should feel therapeutic. If something doesn't feel right, stop and let me know.
The Importance of Posture and Lifestyle Adjustments
Your daily habits significantly impact your sciatic nerve. Small adjustments to how you sit, stand, lift, and sleep can contribute to lasting comfort.
Workplace ergonomics: Ensure your chair supports your lower back, your screen is at eye level, and your feet are flat on the floor.
Proper lifting: Squat down, keep your back straight, and hold objects close to your body. Avoid twisting.
Smart sitting: Take breaks every 30-45 minutes to stand and walk. Use a lumbar support cushion.
Good standing posture: Stand tall with your shoulders back and weight balanced on both feet.
Activity modification: We can help you find smarter ways to do the activities you love without triggering pain.
Sleep positioning: Sleep on your side with a pillow between your knees or on your back with a pillow under your knees to maintain spinal alignment.
Scientific research on conservative treatment confirms that staying active with these changes leads to better outcomes than bed rest.
How a Physical Therapist Creates Your Sciatic Pain Physiotherapy Plan
An effective sciatic pain physiotherapy plan begins with understanding your unique situation, symptoms, and goals.
Our process includes:
Initial assessment: We'll discuss your symptoms, medical history, and how pain affects your life. We also screen for red flags that may require immediate medical attention.
Physical examination: I'll assess your posture, range of motion, strength, and reflexes. We use tests like the straight leg raise to help assess for nerve involvement.
Imaging: X-rays or MRIs are not always needed but may be recommended if pain persists or weakness progresses.
Personalized care plan: Based on the assessment, we develop a plan designed for your specific needs and goals.
Progress monitoring: We regularly check your progress and adjust your plan. Many patients see significant improvement in 4-6 weeks.
Trusted sources and clinical standards we follow
We align our care with respected clinical guidelines and evidence. Explore these resources:
NICE guideline NG59: Low back pain and sciatica in over 16s (https://www.nice.org.uk/guidance/ng59)
American College of Physicians guideline for noninvasive treatments for acute, subacute, and chronic low back pain (https://www.acpjournals.org/doi/10.7326/M16-2367)
NCBI Bookshelf overview on sciatica (https://www.ncbi.nlm.nih.gov/books/NBK507908/)
NHS overview of sciatica symptoms and treatment (https://www.nhs.uk/conditions/sciatica/)
Our team maintains active licensure, pursues ongoing continuing education, and uses outcome measures to track your progress. These standards help ensure your care is safe, effective, and transparent.
When to Seek Professional Help and Your Next Steps
Knowing when to seek professional help for sciatica is critical. While most cases improve with care, some warning signs should not be ignored. Seek immediate medical attention for:
Severe, unbearable pain that doesn't improve with rest.
Progressive weakness or spreading numbness in your leg.
Loss of bladder or bowel control. This indicates a medical emergency called Cauda Equina Syndrome.
Numbness or weakness in both legs, or pain that follows a traumatic injury.
For persistent pain lasting more than a week, professional help is recommended. Early intervention with sciatic pain physiotherapy can help reduce the risk of the condition becoming chronic.
At ChiroHer, we understand how limiting sciatic pain is. We provide award-winning, patient-focused care in Oklahoma City, specializing in providing care for women and prenatal clients. Our team combines chiropractic, acupuncture, and holistic wellness services into a personalized care plan for you.
Don't let sciatic pain control your life. We proudly serve Oklahoma City and the surrounding communities, including Yukon, Edmond, Nichols Hills, Del City, Mustang, and Moore. Our team is ready to help you manage your symptoms.
This guide is for informational purposes and is not a substitute for already established medical advice from your healthcare provider.